By: Joey García | May 14, 2024 | 8 min. read |
Share
Summary of the article The Miami project to cure the paralysis opened its doors to show the work of its researchers to find treatments for spinal cord injury. The open doors included three presentations of doctors and tours of five laboratories at the Christine E. Lynn Rehabilitation Center. Sandra Marin, who came to Miami from Colombia for the Miami project, said that the open doors “offers hope for all with reduced mobility.”
The Miami project to cure the ninth day of open doors of paralysis, and first from the Covid-19 pandemic, presented clarification conversations of the main researchers in the field of spinal cord injury and explored the avant-garde laboratories where researchers are developing innovative therapies.
“We support this open day to link to the people of whom we care so much,” said Barth Green, MD, president and co -founder of the Miami project. “These presentations integrate basic science, engineering and technology by thinking about ways to improve the lives of our patients.”

W. Dalton Dietrich, Ph.D., Scientific Director of the Miami and Dean Senior Dean of Discovery Science at the University of Miami Miller Medicine, gave an overview and highlighted the current and future direction of the center.
“We are a center of neuroscience without borders,” said Dr. Dietrich. “Here, we are developing an infrastructure for the science of clinical translation to protect and repair the nervous system. Our center remains strong, with almost 40 teachers and eight postdocs. We have also been published in hundreds of academic magazines and have $ 19 million in annual funds.”
ESPINAL MEDOL TECHNOLOGY AND INJURIES
The first part of the open doors took place at the Lois Pope Life Center and included three scientific conversations of the main researchers, who presented questions after their presentations.
Patrick D. Ganzer, Ph.D., assistant professor at the Department of Biomedical Engineering at the University of Miami, presented “directed plasticity therapy” and pointed out that therapy uses neuromodulation and bioelectronic medicine to stimulate the peririnal nerve without side effects. This directed approach can easily be turned on and off to affect the vagus nerve. When combined with rehabilitation, therapy is expected to benefit functional recovery after spinal cord injury (SCI).
Hassan A. Ali, Ph.DMSM, associated professor at the Neurological Surgery Department of the Miller School, presented in “Combining Microscopy, Robotics and Automatic Learning to accelerate the discovery of SCI therapy.”

“Developing and discovering drugs is difficult and expensive, which costs $ 2 billion to $ 3 billion per medicine,” said Dr. Ali. “Since my laboratory is involved in test neurons, which can be an intensive labor process, we are finding solutions with avant -garde technologies to relieve the cost by incorporating robots so that the process is more efficient.”
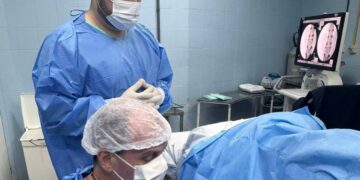
In the final presentation, “brain controlled neuromodulation for neuromotora recovery,” Matija Milosevic, Ph.D., director of neuromotor rehabilitation of the Miami Project, showed how neuromodulation can help improve damaged motor functions, with almost a success rate of 85%. The process is not invasive and focuses on activating electrodes placed on the patient’s skin to increase muscle activity for simple tasks such as sustaining or collecting an article. The objective is to stimulate the column with these same concepts.
Laboratory tours exhibit the last translational science
Open House participants toured the Christine E. Lynn high -end rehabilitation center for the Miami project to cure paralysis in UHEALTH/Jackson Memorial, a comprehensive rehabilitation installation for hospitalized and outpatient patients, and its five laboratories. Anthony CribBs traveled from Oklahoma City with his family to participate.
“Having exhausted the resources available in Oklahoma City, I was anxious to explore the potential that the Miami project has for my progress,” said CribBs, “this event has proven to be incredibly insightful and beneficial. I have had the opportunity to interact with researchers and witness first hand the cutting technology with which they are working.”
Dr. Milosevic’s laboratory members complemented their conference demonstrating that neuromodulation strengthens the connection between the brain and peripheral nerve. Sandra Marin, who came from Colombia to register in the Miami project four months ago, was inspired by work.

“This event offers hope for all of us with reduced mobility,” Marin said. “I was looking for an early perspective in the latest medical practices in Sci and the Miami project is really that place. I have been fortunate to be part of neuromodulation and it has been surprising to see the movement again on my legs, really a wonderful experience.”
Mark Nash, Ph.D., Associate Scientific Director of Research in the Miami Project, directs a laboratory that offered an example of applied physiology, presented by Gary Farkas, Ph.D. Electric currents are directed to metabolism, instead of movement, in the muscles. The approach is important because paralysis increases the risk of metabolic diseases such as obesity and diabetes.
Eva Widerstrom-Noga, Ph.D., research professor at the Department of Neurological Surgery and Physical Medicine and Rehabilitation at Miller School, and her laboratory team is looking to combine therapeutics, including non-pharmacological approaches, to better treat neuropathic pain.
“Today’s approved medication only reduces pain by 33% for one in seven patients,” said Dr. Widerstrom-Noga. “It is important to combine some pharmacological treatments with non -pharmaceutical treatments to reduce this intensity of neuropathic pain. Here, we are using low shock therapy to direct portions of the brain while we work with multisensory integrations.”
Elizabeth Felix, Ph. D., Associated Research Professor in the Department of Physical Medicine and Rehabilitation and Rehabilitation and Project of the Model Model System of the Spinal Media of South Florida, uses another type of shock, quantitative sensory tests, to study paralysis. Its laboratory uses thermal sensitivity tests to investigate why some patients with spinal cord injury experience chronic neuropathic pain.

The tours concluded with an exploration of male fertility, with Emad Ibrahim, MD, assistant professor of urology and neurological surgery at the Miller School and director of the male fertility research program of the Miami project. Dr. Ibrahim showed how the tools for the vibratory stimulation of the penis can help men with SCI who want the father’s children.
“I hope the participants consider that our open doors is interesting and informative,” said Marc Bumoniconti, president of the Miami project. “We are motivated daily to continue our mission as this project changes. Our goal has always been to advance and apply basic translational science. It has been one of the most proud things to be part of.”
Tags: Christine E. Lynn Rehabilitation Center, Dr. Barth Green, Dr. Elizabeth, Dr. Elizabeth Felix, Dr. Emad Ibrahim, Dr. Hassan Ali, Dr. W. Dalton Dietrich III, Eva Widterstrom-Noga, Mark Nash, Miami Project to cure the cure paralysis to cure